Normal reports, persistent symptoms
Normal reports can still sit beside persistent daily disruption.
The dissonance with us is nested deep. What seems reassuring on the surface often still feels unresolved in lived health.

Normal reports can still sit beside persistent daily disruption.
The visible complaint is reviewed while the deeper pattern remains unjoined.
Findings may look improved but the person still feels unresolved in lived health.
Relief may be partial, brief, or followed by another version of the same pattern.
Normal reports, vague explanations, and repeated visits can still leave patients without a clear joined understanding of what is driving the overall pattern.
What is visible in one consultation may not account for regulation, recovery, stress-load, and the subtler shifts that shape how symptoms continue over time.
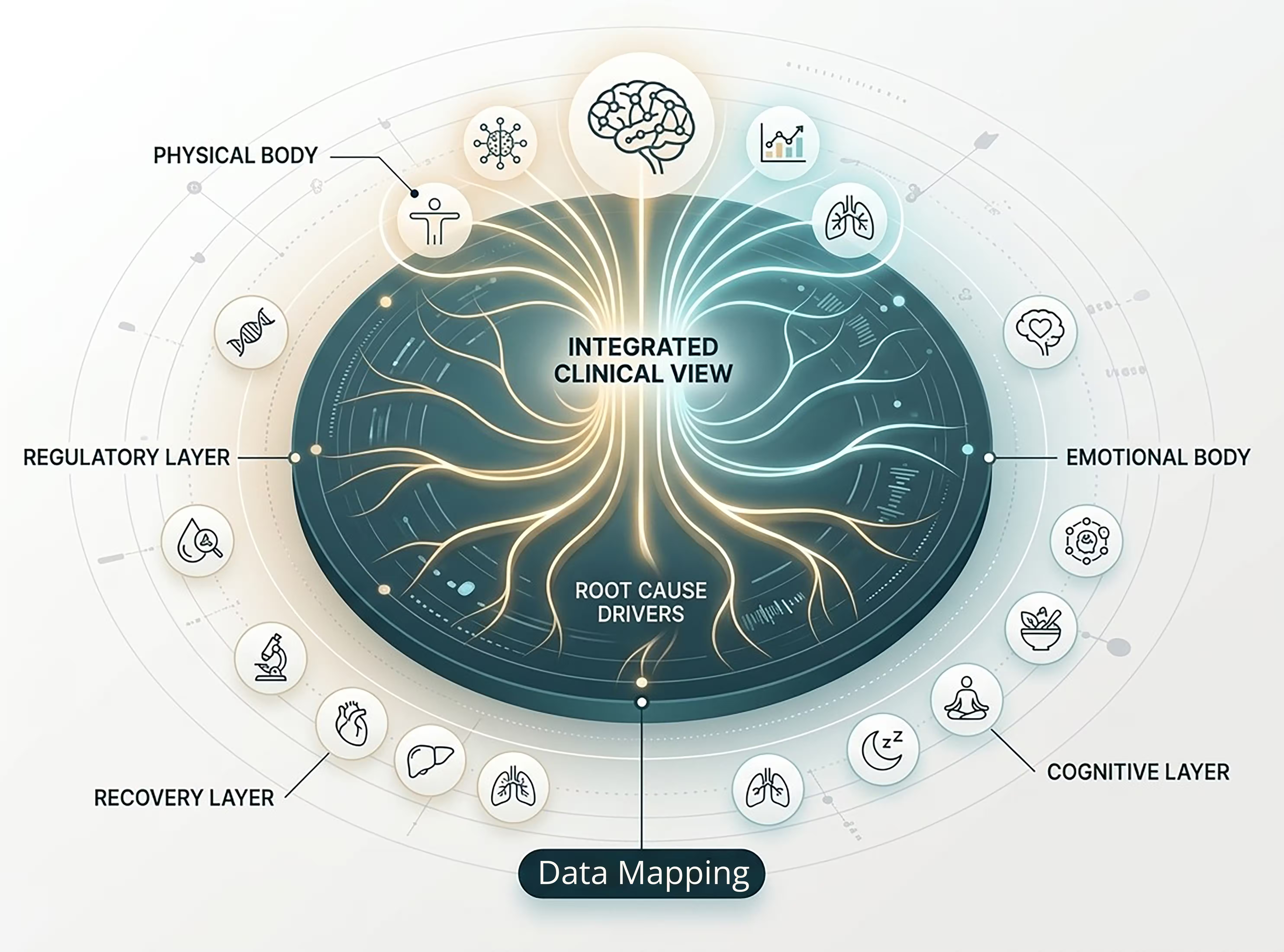
Symptoms can become the visible endpoint of deeper imbalance. This section helps patients understand that what appears first in clinic may not be where the full pattern begins.
Visible symptom burden, structure, medical history, pain, and function.
It organizes what is already visible and gives the assessment a clear physical anchor.
Energy rhythm, resilience, stress load, and adaptation under pressure.
It shows whether the body is maintaining balance or spending too much to stay stable.
Emotional strain, unresolved burden, and the way symptoms intensify around it.
It helps explain why distress and symptoms may keep amplifying each other.
Belief loops, coping style, interpretation patterns, and mental overload.
It reveals internal patterns that may be prolonging fear, confusion, or symptom focus.
Sleep, nourishment, movement tolerance, rhythm, and restoration capacity.
It identifies whether the conditions for healing are present in real daily life.
We begin with the experience before labels become the whole story.
We connect timing, triggers, symptom shifts, and recurring recovery windows.
We trace how systems may influence each other across one broader pattern.
We look for the pressures most likely shaping symptoms, function, and instability.
We build a doctor-led plan with sequence, restraint, and practical clinical clarity.
Special meta with modern clinical medicine.
Special meta with constitution and rhythm support.
Special meta with individualized constitutional reasoning.
Special meta with nourishment, inflammation, and steadiness.
Special meta with regulation and calm under overload.
Special meta with guided resilience and response tracking.
Special meta with supportive dietary and metabolic care.
Special meta with restoration, pacing, and rebuilding capacity.
Special meta with doctor-led integration and sequencing.
Special meta with sensory and nervous-system support.
Focus areas where broader root understanding often becomes clinically useful.
Focus asks chronic conditions where long adaptation and load are visible.
Focus conditions where inflammation and deeper immune patterning both matter.
Focus stress, overload, and the body-mind interaction around symptoms.
Focus rhythm, endocrine strain, metabolism, and cycle imbalance.
Focus chronic instability, nutrition load, and emotional relation.
Focus biomarkers, repeated patterns, and immune-linked variation.
Focus adaptive shifts, energy changes, and rhythm disorders.
Focus patterns where neural adaptation or reactive strain keeps returning.
We bring together clinical grounding, systems thinking, and personalized interpretation so persistent symptoms can be read with more context and less fragmentation.
Doctor credibility
Lead doctor insight
Personalized care

Begin from the person and the lived story, not only from the report.
Build a wider view so symptoms, triggers, and recovery can be read together.
Direction is selected with context, pacing, and clinical restraint.
Signals are followed across adaptation, stability, and lived response.
Care evolves as the body shows what is actually changing in function, resilience, and recovery.
From repeated short-term confusion toward clearer, more integrated direction.
The clearest change was finally understanding why the body kept cycling between better days and crashes.A.R. What changed
This changed the way recurring problems were seen because the full story was discussed together.R.S. What changed
The biggest relief was understanding that symptoms and lived distress were connected, not random.N.M. What changed
Patient stories use initials only and are shared in non-promissory form.
Why normal reports do not always mean the full picture is normal.
How similar symptoms can still point to different patterns and different care.
What integrated medicine means when it stays clinically grounded and responsible.
ROOTOPATHY is a root-first clinical approach that looks beyond isolated symptoms to understand the deeper pattern shaping health, stress, recovery, and chronic imbalance.
No. It is designed to work alongside responsible evidence-informed care, and it does not replace emergency treatment, statutory care, or necessary specialist medical support.
It is often helpful for people with persistent symptoms, recurring health patterns, post-illness depletion, or situations where reports exist but the full picture still feels incomplete.
The assessment looks at symptoms, health history, stress load, recovery patterns, and broader system signals so care can begin from a more complete clinical picture.
If you have reports, prescriptions, or past diagnoses, they can be helpful. If not, the consultation can still begin from your history, symptoms, and present concerns.
It is most often useful where patterns are persistent, recurring, or unclear, but the deeper root-based framework can also help when recovery feels incomplete or fragmented.